Polycystic Ovarian Syndrome Symptoms, Causes, Diagnosis and Treatment | PCOS
PCOS is a disease that affects the ovaries, disrupting the normal ovulation process due to a hormonal imbalance. It is sometimes accompanied by several symptoms that appear together in the patient, in which case it is called polycystic ovary syndrome. These symptoms include menstrual irregularities and weight gain, appearance of coarse hair in different areas of a woman's body are symptoms, and sometimes the disease is asymptomatic and may be discovered incidentally during a routine examination.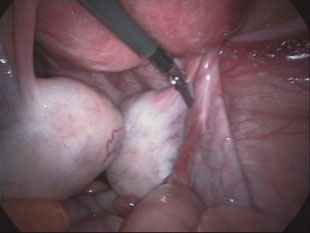
Prevalence and incidence of polycystic ovary syndrome (PCOS): It is a very common gynecological condition, and the incidence varies from country to country, and the overall infection rate ranges from 5-10%, and this rate is increasing without knowing the reasons
Causes of polycystic ovary syndrome (PCOS):
The true causes of the disease are unknown. It is believed that there is a genetic component to the disease, and it is believed that the gene is of the dominant type. Its appearance in women is associated with male-pattern baldness in women, and the genetic inheritance of the disease has not yet been discovered. The age group most affected by this condition is adolescence, a time marked by rapid weight gain and hormonal changes.
Some studies suggest a link between insulin receptor function and certain medications, such as some epilepsy treatments, can cause these symptoms in users.
Symptoms of Polycystic Ovary Syndrome (PCOS):
As previously mentioned, the symptoms of this condition vary greatly and can sometimes be discovered incidentally during a routine examination. Diagnosis is based on an ultrasound image of the ovaries, which reveals the presence of 10-12 follicles measuring 8-10 mm distributed around the periphery of the ovary.
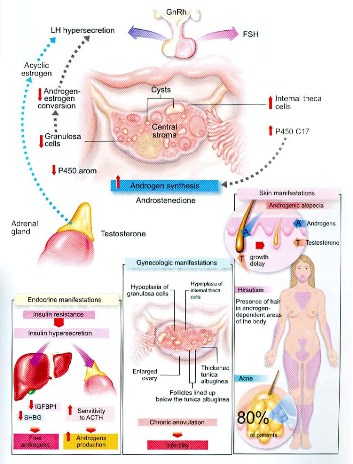
Other symptoms include:
1- Menstrual cycle disturbances, which come in the form of amenorrhea or infrequent periods. The amenorrhea may be primary or secondary depending on the severity of the disease.
2- Weakness and disturbance in the ovulation process, which leads to delayed pregnancy and cases of primary or secondary infertility.
3- Weight gain, with the patient's BMI > 30 kg. The weight gain is usually concentrated in the trunk and limbs, and this occurs due to an imbalance in the body's lipid levels, including leptin.
4- The appearance of coarse hair in various areas of the woman's body, including the chin, upper lip area, lower abdomen, and chest. This occurs as a result of an imbalance in male hormones.
5- Increased risk of acne and oily skin.
6- Recurrent miscarriages due to elevated LH hormone levels.
7- Polycystic ovary syndrome (PCOS) may be associated with high blood pressure and diabetes.
8- It can also lead to depression or other psychological problems
Causes of these symptoms:
The hormonal changes that occur in polycystic ovary syndrome (PCOS) are not fully understood, but the most important factor is elevated insulin levels in more than 50% of cases. This hormone is secreted by the pancreas, and its primary function is to bind to the cell membrane It then carries glucose molecules from the blood into the cells, where they are used to produce energy and carry out metabolic processes.
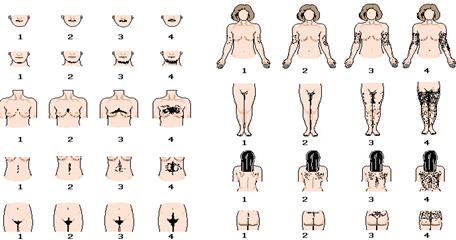
However, in polycystic ovary syndrome (PCOS), these molecules are unable to perform this function despite their normal adhesion to the cell wall, which in turn signals the pancreas to The hormone is secreted to compensate for the decreased effectiveness, thus increasing hormone levels.
This effect on the ovaries can be summarized in two main points:
1- A disruption in the ovaries' response to hormonal signals from the brain responsible for egg production, leading to premature cessation of egg development and their retention in the ovaries as small, adjacent cysts.
-
Increased secretion of male hormones from the ovaries, as well as increased sensitivity of body cells to these hormones.
Diagnosis of Polycystic Ovary Syndrome (PCOS): Diagnosing the disease is not difficult nowadays and depends on three factors:
First: A physical examination of the patient and observation of the symptoms mentioned previously.
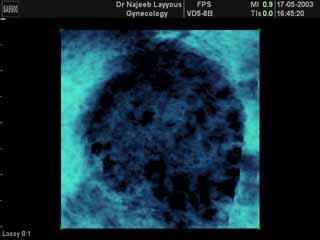
Second: Some laboratory tests include:
1- Elevated LH hormone levels
2- Elevated insulin levels despite normal blood sugar levels. This is due to ineffective insulin receptors, leading to increased insulin secretion.
3- Elevated testosterone levels.
4- Elevated prolactin levels
5- Elevated estradiol and estrone levels.
6-- Decreased levels of sex hormone receptors.
7- Sometimes the disease is accompanied by thyroid hormone and prolactin hormone imbalances.
Third: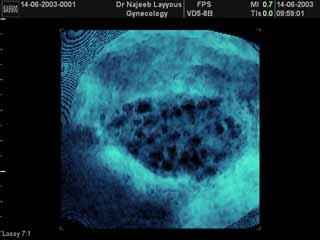
The best way to diagnose the condition is by performing an abdominal or vaginal ultrasound. The vaginal ultrasound is preferred due to its accuracy, reaching 100%, while the abdominal ultrasound has a 30% error rate. The visual finding is the appearance of 10-12 small cysts ,More than 8-10 mm in size, distributed in a ring-like pattern resembling a string of pearls, there is also an enlargement of the ovary, increasing its size by one and a half to three times its normal size, and an increased concentration of ovarian tissue is observed in the center.
Treatment of polycystic ovary syndrome (PCOS):
Treatment for PCOS focuses on managing its symptoms, as there is no cure for the disease.
First: Menstrual cycle irregularities: This can be treated by using birth control pills or progesterone pills regularly, along with metformin pills at a dosage appropriate to the patient's weight, and continuing to take them until the body's hormones are regulated.
Secondly: The appearance of coarse hair: This is achieved by taking anti-androgen pills, but these treatments require a period of 6-8 months for changes in hair thickness to occur. Therefore, it is recommended to use other methods of hair removal until these treatments begin to work, such as laser hair removal and the use of various hair removal products
Third: Weight gain,There is a very strong link between weight gain and the disease, and both lead to each other, as weight gain can be associated with a hormonal imbalance, which in turn leads to polycystic ovary syndrome (PCOS), and vice versa. It is highly recommended to use dietary programs and exercise to reduce weight in order to balance this hormonal imbalance.
The benefits of weight loss include:
- Reduced insulin resistance
- Reduced risk of heart disease
- Reduced risk of uterine cancer
- More regular menstrual cycles
- Increased chances of pregnancy
- Reduced acne and excess hair growth
- Improved mood.
Fourth: Infertility: Infertility treatment is divided into two types:
1- Drug therapy 2- Surgical treatment
-Drug therapy for polycystic ovary syndrome (PCOS):
Drug treatments are also divided into two categories:
The first type is Metformin pills, which help regulate the body’s hormones and increase the ovaries’ response to stimulating treatments. This treatment also helps prevent an excessive response when using ovulation-stimulating injections or pills. It is also recommended to use these pills during the first months of pregnancy to reduce the rate of miscarriage during this period.
The second treatment is to give the patient ovulation-inducing hormones, either in the form of Clomid pills or FSH/LH hormone injections, with careful monitoring of the ovaries and identification of ovulation days. When ovulation occurs, the chance of pregnancy is about 40%.
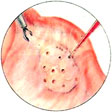
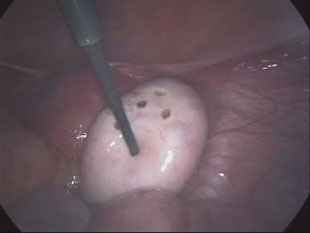
Surgical treatment for polycystic ovary syndrome (PCOS):
The old surgical method for ovarian surgery involved the surgical removal of part of the ovaries. This required opening the patient's abdomen, which could result in adhesions that, in turn, led to infertility. This procedure is no longer used today.
Long-term complications of polycystic ovary syndrome (PCOS):
1. Diabetes.
2. Uterine cancer.
3. High blood pressure.
4. Certain cardiovascular diseases.
5. Lipid disorders and excess fat in the body.
What can be done to reduce long-term health risks?
- Adopt a healthy lifestyle (a balanced diet, regular exercise, and weight loss).
- Get regular medical checkups to avoid the risk of developing conditions such as diabetes, high blood pressure, and endometriosis.
The New Revolution in Women's Health 2026-May
Goodbye PCOS... Hello PMOS
After more than 90 years, science has finally agreed that the term "Polycystic Ovarian Syndrome" was misleading. In May 2026, by decision of 56 international medical organizations and published in The Lancet, the name was officially changed to:
Polyendocrine Metabolic Ovarian Syndrome (PMOS).
Why this change now?
Because the old focus on "cysts" was wrong; what appears on ultrasound are not true cysts but rather "follicles" that have stopped growing. More importantly, PMOS is not just an ovarian disease, but a comprehensive "systemic" disorder that affects ovulation, the reproductive system, insulin, metabolism, skin, and even mental health.
The Four Dimensions of PMOS: What Does the Patient Experience?
The condition must be assessed from four integrated perspectives:
Reproductive dimension: Impaired egg maturation leads to delayed pregnancy and menstrual irregularities.
Metabolic dimension: 70% of patients have insulin resistance, increasing the risk of diabetes fourfold.
Endocrine dimension: Elevated male hormones (androgens) cause hirsutism and acne.
Psychological dimension: Our deep understanding that PMOS increases anxiety and depression necessitates compassionate and supportive care.
How do we diagnose PMOS?
Modern diagnosis does not require the presence of all symptoms. Instead, we rely on precise criteria that include:
Menstrual irregularities: (fewer than 8 periods per year).
Signs of hyperandrogenism: such as resistant cystic acne or unwanted hair growth.
Ultrasound: Using the latest technology to precisely visualize the follicular units (12-25 follicles).
Treatment Roadmap: An Individualized, Goal-Based Approach
We believe that every patient is unique, so we design a treatment plan based on your health goals and age:
Lifestyle Modification (Cornerstone): We begin with a personalized lifestyle program. Science has proven that losing just 5-10% of body weight restores ovulation in 80% of patients, a more powerful effect than any medication in improving insulin sensitivity.
Cycle Regulation and Endometrial Protection: We use combined oral contraceptives or cyclical progesterone to ensure endometrial regulation and prevent future hyperplasia.
Ovulation Stimulation for Those Wishing to Conceive: We use ovulation-inducing medications at carefully calculated doses to suit each individual case.
Insulin Resistance Treatment: We use the Metformin protocol (1500-2000 mg daily) to improve metabolism, reduce the risk of diabetes, and decrease the rate of early miscarriage.
Beauty and Skin Solutions: We address hirsutism and acne with anti-androgen medications that block receptors, giving you the skin you deserve. Our vision: Protecting your future health.
Changing PCOS name to PMOS confirms the validity of our long-standing protocol, which focuses on "long-term follow-up." We are committed to a follow-up protocol that includes:
Regular glucose and lipid tolerance testing to protect your heart and regulate your metabolism.
Endometrial ultrasound assessment if you have been amenorrhea for more than 3 months.
Ongoing psychological support, because we believe that psychological well-being is key to hormonal balance.
PMOS is not just a new name; it's a promise to provide deeper, more comprehensive medical care. We are here to transform this hormonal challenge into a journey of success and restored confidence.
Dr Najeeb Layyous F.R.C.O.G
Consultant Obstetrician, Gynecologist and Infertility Specialist


 Pregnancy Due Date Calculator
Pregnancy Due Date Calculator
 Chinese Gender Predictor
Chinese Gender Predictor
 Ovulation Calculator
Ovulation Calculator
 IVF Due Date Calculator
IVF Due Date Calculator
